Spinal Cord Injuries, Percutaneous Discectomy & Other Possible Treatments
Survivors of major car accidents and catastrophic falls must regularly seek out the best medical treatment they can afford for their pain and injuries explains a New York City spinal cord injury lawyer at the F&A accident law firm. At present, car accidents cause over 35 percent (35%) of all new spinal cord injuries (SCIs) and another 10% of them are due to motorcycle, bicycle, and ATV accidents.
Falls from higher levels account for 81% of all fatal falls. Taken together, workplace falls and those occurring elsewhere directly cause 25% of all new spinal cord injuries.
Depending on the severity of your injuries, you may first see a chiropractor or orthopedic surgeon for evaluation. While initial treatments may include physical therapy, nerve blocks, and prescriptions for opioids and other pain killers, your doctor may soon suggest steroid injections – or an outpatient surgical procedure to relieve pain known as a percutaneous discectomy.
Here’s a closer look at what this procedure entails – along with a brief review of other surgeries or procedures that your main doctor or pain management specialist may believe are better suited to your injuries and needs.
What is a Percutaneous Discectomy and How Is It Performed?
Before performing this outpatient procedure (requiring local anesthesia) to relieve pressure on your spinal nerves, your doctor will normally inform you about the following facts regarding your spine.
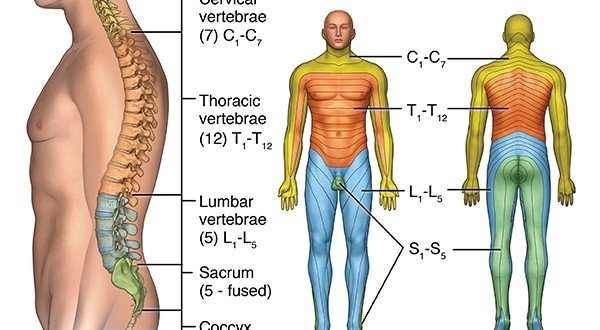
- Your spine consists of bony vertebrae. In between the different vertebrae, there are soft structures known as discs. When you’re young and those discs are still healthy, they operate like shock absorbers between the vertebrae;
- Worn out and damaged discs often cause pain. If you develop a herniated disc, this usually means that part of the substance that normally stays inside the disc has started bulging outwards – putting major pressure on one or more nearby nerves. In many cases, that pressure can cause pain to radiate down into your back, legs, neck, or arms (often referred to as radiculopathy).
Percutaneous discectomy is the treatment used to reduce this disc swelling or inflammation. It involves introducing a needle into the disc and removing the excess fluid. By using a process called fluoroscopy (live X-ray), your doctor can guide the needle into the disc. Next, a probe including a rotating tip is inserted into the needle. With the probe turned on, the rotating tip is used to remove small amounts of the disc nucleus. Since this empty space in the disc is relatively small, the disc and spine normally remain stable.
While this straightforward procedure normally just takes less than an hour, a small percentage of doctors still perform it negligently — causing patients to suffer moderate to severe injuries.
Possible Complications Following a Percutaneous Discectomy
All invasive medical procedures involving the spinal cord can prove risky, even those performed using a needle and less aggressive surgical techniques. Some of the most common complications include:
- Permanent, increased pain near the disc site, often radiating elsewhere (radiculopathy);
- Nerve damage;
- Increased intracranial pressure;
- Unusual bleeding or formation of a blood clot;
- Spinal cord compression;
- Paralysis and/or new types of numbness in one or more extremities; and
- Infection and improper wound healing where the needle was introduced into the body
Patients who were not properly screened by their surgeons in advance may also suffer additional spinal damage if they were already suffering from a condition like spinal stenosis – or some of their disc material was already present in the spinal canal.
Depending on Your Specific Spinal Injuries, Other Procedures/Treatments May Be Suggested
- Spinal fusion. This type of surgery is considered one of the most common approaches to relieving back pain. While performing this procedure, your surgeon will join your vertebrae (spinal bones) together. In advance, you’ll be told exactly how this procedure may limit certain motions and how far different nerves may have to stretch. In some cases, the bones may not fuse properly;
- During this procedure, your doctor will remove the bone spurs – or parts of the bones in your back. This can help relieve some of the pressure on nearby spinal nerves, easing your pain and discomfort. However, your spine may become less stable, requiring a later spinal fusion procedure;
- This surgery requires your physician to cut away and remove bone on the sides of your vertebrae – hoping this will widen the space where your nerves leave your spine. This process can help relieve pressure on the nerves and diminish your pain. However, like the laminectomy, this surgery can destabilize your spine – increasing the possibility that you’ll need a later spinal fusion;
- Interlaminar implant. During this process, your surgeon will implant a U-shaped device between two of your vertebrae – normally easing the pressure in that region. In some cases, this is done at the same time as a laminectomy (see above). Normal problems after this procedure involve a limited range of motion when trying to bend backward using this part of the spine;
- Disc replacement. Once the damaged disc is removed, an artificial one is inserted between your vertebrae. While recovery time may be shorter for this procedure, this new disk can fall out or slip out of place, requiring follow-up surgery.
If you or a loved one has suffered serious pain or a worsening of your spinal cord injury or condition following any of the surgeries or procedures described above – be sure to contact your New York spinal cord injury attorney right away.